PRP Hair Therapy in Kent: What It Is and How It Works
- Juvenology Clinic

- 2 days ago
- 11 min read
There are treatments in aesthetic medicine that work by substitution: filling what has been lost, relaxing what has contracted, covering what has changed. And there are treatments that work by something closer to instruction, delivering a biological signal that tells the body to repair itself.
PRP is in the second category. Understanding that distinction is the starting point for understanding what it can and cannot do, who it is genuinely suited to, and why it occupies a specific and important position in the regenerative treatment toolkit at Juvenology.
This post covers what platelet-rich plasma actually is at a biological level, the specific growth factors responsible for its clinical effects, what those effects mean in practice for hair and skin, what the evidence says about outcomes, and how the assessment at Juvenology determines whether it belongs in your treatment plan.

What PRP actually is
Platelet-rich plasma is not a drug, a product, or a substance introduced from outside the body. It is a concentration of your own blood, specifically the platelet-rich fraction, prepared in a way that amplifies the biological signals your platelets naturally release when tissue needs to repair itself.
The process begins with a straightforward blood draw from your arm. That blood is placed in a centrifuge and spun at a controlled speed that separates the components by density. Red blood cells, which are heavy, settle at the bottom. Platelet-poor plasma, which is lighter, sits above them. Between these layers, the fraction we are interested in, is the platelet-rich plasma: a concentrated layer containing 5 to 10 times the normal platelet concentration found in circulating blood.
That concentrated fraction is then activated, either by the introduction of calcium chloride or by exposure to the tissue environment itself, which causes the platelets to degranulate and release their contents. What they release is the reason PRP works.
In cardiac nursing, platelet biology is not an abstract concept. It is foundational clinical knowledge. We understood platelet aggregation, degranulation, and the coagulation cascade because managing them in high-acuity cardiac patients was part of daily practice. That background is part of why PRP's mechanism made immediate sense to me when I encountered it in aesthetic medicine: this is not a novel intervention. It is a precision application of a biological system I had worked with for fifteen years.
The growth factors, and what each one does
Platelets exist in the bloodstream to orchestrate tissue repair. When a blood vessel is injured, platelets aggregate at the site and release a cascade of signalling proteins, growth factors, that recruit cells to the area, initiate proliferation, stimulate collagen synthesis, and promote the formation of new blood vessels. This is the body's first-responder repair system, refined over millions of years of evolution.
PRP harnesses this system by delivering those same growth factors at a concentration significantly above baseline, directly into the tissue that needs repair. The primary growth factors and their specific roles are worth understanding because they explain why PRP produces the results it does, and why it produces them gradually rather than immediately.
Growth Factor | Primary Biological Role | Clinical Effect in Hair | Clinical Effect in Skin |
PDGF (Platelet-Derived Growth Factor) | Stimulates cell proliferation and tissue repair | Activates dermal papilla cells and supports follicle regeneration | Stimulates fibroblasts to produce collagen and extracellular matrix |
VEGF (Vascular Endothelial Growth Factor) | Promotes angiogenesis (new blood vessel formation) | Improves follicular blood supply and nutrient delivery | Enhances skin vascularity and tissue vitality |
TGF-β (Transforming Growth Factor Beta) | Modulates inflammation and tissue remodelling | Reduces inflammatory signals linked to follicular miniaturisation | Reduces chronic inflammatory ageing processes |
FGF (Fibroblast Growth Factor) | Supports cell growth and regeneration | Extends the anagen (growth) phase of hair | Stimulates keratinocyte renewal and barrier repair |
IGF-1 (Insulin-Like Growth Factor 1) | Promotes cell survival and inhibits apoptosis | Helps preserve follicular viability | Supports dermal repair and tissue resilience |
PDGF is the primary driver of cell proliferation. It recruits fibroblasts to the treated area and stimulates them to divide and produce collagen and extracellular matrix. In the scalp, PDGF activates dermal papilla cells, the cells at the base of each hair follicle that determine whether a follicle grows a terminal or miniaturised hair.
VEGF drives angiogenesis, the formation of new blood vessels. In the scalp this is critically important: follicles that are miniaturising do so partly because their blood supply has diminished. VEGF improves microcirculation at the follicular level, restoring the nutrient and oxygen delivery that healthy follicular activity requires. In the skin, improved vascularisation improves tissue quality and the speed of the regenerative response.
TGF-β modulates the inflammatory environment. TGF-β suppresses pro-inflammatory cytokines including IL-6 and TNF-α, the inflammatory signals that contribute to follicular miniaturisation in androgenetic alopecia and to the chronic low-grade inflammation that accelerates skin ageing. PRP is not only regenerative. It is anti-inflammatory.
FGF extends the anagen phase of the hair growth cycle, the active growth phase during which the follicle is producing a hair shaft. In skin, FGF stimulates keratinocyte proliferation, supporting epidermal renewal and barrier function.
IGF-1 promotes cell survival and inhibits apoptosis, programmed cell death, in follicular cells. Follicles that are miniaturising are progressively moving toward a state where their cells can no longer sustain themselves. IGF-1 counteracts that trajectory.
PRP for hair: what the evidence says
Hair loss is the most extensively studied application of PRP in aesthetic medicine, and the evidence base has matured considerably over the last three years. The signal across the literature is consistent and clinically meaningful, though it comes with important caveats about patient selection and what PRP is and is not appropriate for.
Study | Year | Key Findings |
British Journal of Dermatology Systematic Review | 2025 | 30–40% increase in hair density after 3–6 months; 70–80% response rate |
Meta-analysis in Female Androgenetic Alopecia | 2024 | Significant improvement in density and hair shaft thickness |
Meta-analysis of 864 Patients | 2023 | Activated PRP shown to be safe and effective for terminal hair density |
PMC Mechanism Review | 2025 | Confirmed PRP acts through multiple simultaneous regenerative pathways |
A 2025 systematic review published in British Journal of Dermatology found that PRP produces a 30 to 40% increase in hair density after three to six months of treatment, with 70 to 80% of patients responding when treatment follows established protocols. The review also confirmed a 76% patient satisfaction rate, a figure that reflects what happens when appropriate candidates receive treatment for the right indication.
What PRP does biologically in the scalp, extending the anagen phase, improving follicular microcirculation, reducing inflammatory signals, stimulating dermal papilla cells, translates clinically to reduced shedding, improved hair thickness, and in many patients meaningful regrowth in areas of active thinning where viable follicles still exist beneath the surface.
That last phrase carries the most important clinical caveat. PRP works by reactivating follicles that are dormant or miniaturising. It cannot regenerate follicles that have been fully replaced by scar tissue or that have been absent for many years. This is why timing and candidacy assessment matter. Earlier treatment consistently produces better outcomes because there is more viable follicular tissue to work with. I see this pattern consistently in clinic: the patients who respond most dramatically are those who came in early, before the thinning became advanced enough to narrow the treatment's options significantly.

Results from the Juvenology treatment room
These are real patients treated at Juvenology. No filters, no editing. All four cases show hair PRP results across different patient profiles, different degrees of thinning, different hair types, and different clinical goals. What they share is that each patient had viable follicular tissue to work with, which is the single most important determinant of how well PRP performs.
The early male intervention
This patient presented with androgenetic alopecia in its earlier stages, visible as a receding and thinning frontal hairline with the scalp increasingly visible through the hair at the front of the head. The hair itself retained good calibre in the existing shafts, which indicated that follicular miniaturisation was underway but not advanced. The scalp was visible through the hair when viewed from above and from the side.

The after image shows a meaningfully denser frontal zone. The hairline has not been surgically repositioned, but the hair in the existing hairline zone is noticeably thicker and more numerous, with new terminal hairs visible along the frontal edge where fine, sparse hairs were present before. The scalp visibility through the frontal hair has reduced significantly. This is the result that PRP produces most consistently in earlier-stage male androgenetic alopecia: not dramatic hairline restoration, but meaningful improvement in density and hair calibre in the zones where follicles are miniaturising rather than absent.
Female diffuse thinning at the crown
This patient presented with diffuse thinning concentrated at the central parting and crown, a pattern consistent with female pattern hair loss. The before image shows a wide, visible parting with the scalp clearly visible along the central line and extending toward the front of the head. The existing hair had reasonable shaft calibre but insufficient density to cover the scalp at the parting zone.

The after image shows a noticeably reduced parting width, with new hair growth filling in along the central parting and crown. The scalp is significantly less visible and the hair appears fuller and denser throughout the top of the head. This is a strong clinical result for female pattern thinning and reflects what PRP does most effectively in this presentation: reactivating dormant follicles along the parting zone and increasing the density of existing terminal hairs through improved follicular microcirculation and reduced miniaturisation signalling.
The established male case
This patient presented with more advanced androgenetic alopecia, with significant diffuse thinning across the entire top of the scalp and the frontal zone. The scalp was clearly and extensively visible through sparse, fine hairs across a wide area. This patient sat toward the upper end of what PRP can realistically address, and the clinical conversation at consultation included honest expectation-setting about the degree of improvement achievable versus what surgical hair restoration would produce.

The after image shows meaningful improvement across the treated zone. The hair is noticeably denser, the scalp less visible, and the existing hairs appear thicker and more substantial. This is not a complete reversal of the thinning, which was never the clinical goal for a case at this stage, but a visible and clinically significant improvement in density that has meaningfully changed the appearance of the scalp. It demonstrates what PRP can achieve even in more established cases when follicular tissue is still present and responsive.
Female thinning at the parting
This patient presented with thinning concentrated along the central parting rather than diffuse thinning across the whole crown. The before image shows a wide parting with the scalp visible along the central line, but good density and volume in the surrounding hair. The contrast between the sparse parting zone and the fuller surrounding hair made the thinning visually prominent despite the overall hair volume being reasonable.

The after image shows a noticeably narrower parting, with new hair growth filling the zone along the central line and significantly reducing scalp visibility. The density improvement is concentrated exactly where it was needed, along the parting, rather than producing a generalised change across the whole head. The hair volume and quality in the surrounding areas appears maintained. This is a precise result that reflects how PRP performs when the thinning is localised and the follicular tissue in the affected zone is still viable and responsive.
What PRP will not do
Being precise about the boundaries of PRP's clinical utility is as important as describing what it does. Patients who arrive expecting PRP to add volume, produce immediate dramatic change, or address structural concerns like significant skin laxity will be disappointed. Not because the treatment failed, but because those are not the problems PRP is designed to solve.
PRP is a regenerative treatment that works through the body's own biological processes. Results develop gradually over three to six months as collagen synthesis builds and the tissue remodels. The result at six months is typically better than the result at six weeks, the opposite of filler or toxin where the result is visible immediately. Expecting an immediate transformation after PRP is a mismatch of expectations with mechanism.
PRP does not add volume. For patients whose primary concern is facial hollowing, dermal fillers address that directly.
PRP does not lift descended tissue. For patients with significant facial laxity, HIFU skin tightening or PDO threads are more appropriate first-line interventions.
For hair loss driven by a systemic cause, hormonal decline, nutritional deficiency, thyroid dysfunction, high inflammatory burden, PRP alone will not address the driver. This is why the assessment at Juvenology always considers the systemic picture before recommending treatment. Our Advanced Blood Panel identifies the hormonal and metabolic factors that may be contributing to the thinning, and where those factors are present, addressing them through Longevity Medicine alongside the PRP course produces outcomes that PRP in isolation cannot achieve.
PRP is a protocol, not a procedure.
PRP Combination Treatments
Combination | Why They Work Well Together |
PRP + Microneedling | Enhances growth factor penetration and collagen stimulation |
PRP + Polynucleotides | Combines growth factor signalling with DNA-based tissue repair |
PRP + Longevity Medicine | Addresses systemic drivers affecting tissue regeneration |
PRP + Hair Loss Medical Therapy | Supports follicle biology alongside pharmacological stabilisation |
Who is a good candidate
PRP is most appropriate for patients with the following presentations.
For hair: patients experiencing androgenetic alopecia in its earlier to moderate stages, patients with telogen effluvium following hormonal change, physical stress, or illness, and patients with diffuse thinning where viable follicles are still present beneath the surface. The earlier the intervention, the more follicular tissue there is to work with and the more pronounced the response.
Ideal Candidate | Why PRP Works Well |
Early to moderate androgenetic alopecia | Viable follicles still present |
Diffuse thinning after stress or illness | PRP supports follicular recovery |
Patients with dull or thinning skin | Stimulates collagen and vascular repair |
Patients wanting natural regenerative improvement | Uses the body’s own repair signals |
Patients willing to commit to a treatment course | Results build progressively over time |
For skin: patients seeking improvement in overall skin quality, texture, luminosity, fine lines, pore appearance, and the gradual dermal thickening that produces more resilient and vital-looking skin. Patients combining PRP with polynucleotides often achieve a more comprehensive result than either treatment alone, with each working through a distinct regenerative mechanism: PRP through growth factor stimulation, polynucleotides through the adenosine receptor pathway.
For both: patients who understand that results develop over months rather than days, and who are committing to a course of treatment rather than a one-off intervention.
What a PRP consultation at Juvenology involves
Every PRP consultation begins with a clinical assessment of what is driving the concern. Because PRP is not the right starting point for every patient who presents with hair thinning or skin quality concerns.
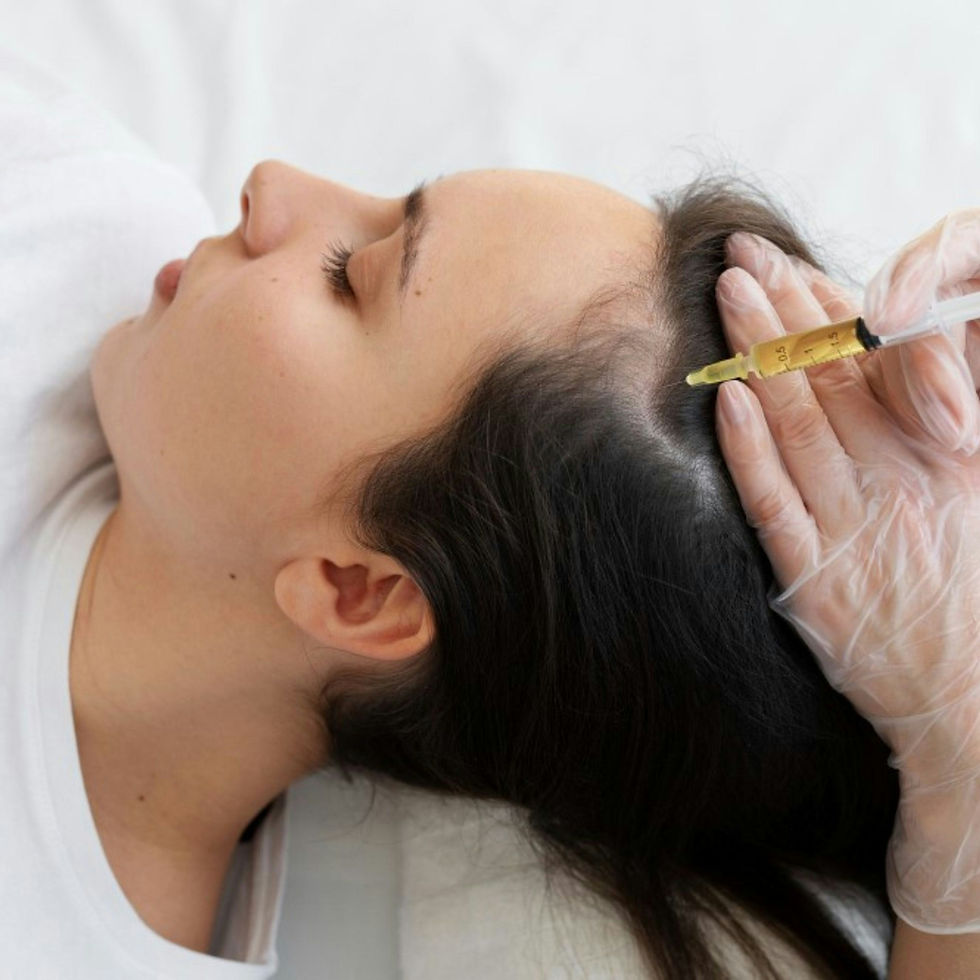
For hair patients, I assess the pattern and degree of thinning, the timeline, and any associated symptoms that suggest a systemic driver. Where the history suggests hormonal, thyroid, or inflammatory factors, I recommend the Advanced Blood Panel before beginning treatment. A PRP course that runs alongside unaddressed hormonal decline will produce weaker and less sustained results than one conducted in an optimised systemic environment. This is not a caveat I add reluctantly. It is a clinical reality I see directly in the outcomes.
I do not recommend PRP to every patient who asks about it. The consultation is where I determine whether it is the right tool for your specific concern. If something else would serve you better, I will tell you that directly.
PRP is one of the most honest treatments in aesthetic medicine. It doesn't pretend to do things it can't. It delivers your own growth factors to tissue that needs regenerative stimulus, and then it steps back and lets your biology do the work. When the candidate is right and the systemic environment is optimised, the results reflect that. When the indication is wrong, no concentration of platelets will compensate. The consultation is where we work out which category you fall into.
To discuss whether PRP is appropriate for your hair or skin concern, book a consultation at Juvenology.
We see patients from across Kent including Maidstone, Tonbridge, Sevenoaks, Kings Hill, West Malling, Medway, and Chatham.
About the author

Nurse Marina is the founder of Juvenology Clinic in Maidstone, Kent.
She spent 25 years in nursing, including six years as a cardiac nurse at KIMS Hospital, before founding Juvenology to combine regenerative aesthetic medicine with longevity science.
She holds an Executive MSc in Longevity from the Geneva College of Longevity Science, has completed the Healthy Longevity Clinician Programme at the National University of Singapore, and holds qualifications in hormonal health from the Marion Gluck Academy.
She is NMC Registered, JCCP Verified, BACN Member, ACE Group Registered, a Member of the Royal College of Nursing, and recognised by the Professional Standards Authority.
Clinical references
Platelet-Rich Plasma (PRP): Molecular Mechanisms, Actions and Clinical Applications — PMC, 2025 ncbi.nlm.nih.gov/pmc/articles/PMC12608683
Inflammatory Signatures and Biological Markers in PRP Therapy for Hair Regrowth: Comprehensive Narrative Analysis — PMC, 2025 ncbi.nlm.nih.gov/pmc/articles/PMC12071426
PRP Effectiveness in Treating Androgenetic Alopecia: Comprehensive Evaluation — PMC, 2025 pmc.ncbi.nlm.nih.gov/articles/PMC11817460
PRP in Dermatology: Cellular and Molecular Mechanisms of Action — PMC / Biomedicines, 2024 ncbi.nlm.nih.gov/pmc/articles/PMC10813350
Use of Platelet Rich Plasma for Skin Rejuvenation — Skin Research and Technology / Wiley, 2024 onlinelibrary.wiley.com/doi/10.1111/srt.13714
PRP in Facial Rejuvenation: Systematic Appraisal of Available Clinical Evidence — PMC pmc.ncbi.nlm.nih.gov/articles/PMC8606573
PRP Effectiveness for Hair Loss: Complete Scientific Review 2025 — The Wellness London thewellnesslondon.com/articles/how-effective-is-prp-for-hair-loss-a-complete-scientific-review-in-2025